 Millions of Americans are in pain and looking for non-opioid pain treatments to manage their chronic pain while avoiding the side effects and addiction of opioids. Fortunately, there are several non-opioid (non-narcotic) pain treatments available for pain management at Novus Spine & Pain Center in Lakeland, Florida.
Millions of Americans are in pain and looking for non-opioid pain treatments to manage their chronic pain while avoiding the side effects and addiction of opioids. Fortunately, there are several non-opioid (non-narcotic) pain treatments available for pain management at Novus Spine & Pain Center in Lakeland, Florida.
What Are Non-Opioid Pain Treatments? Why Are They Important?
Non-opioid pain treatment is one that does not make use of opioids (narcotics), avoiding the negative and addictive effects associated with opioids.
It is important to know that opioids can reduce some types of pain, but not all types of pain. In some cases, opioids may increase the perceived intensity of pain. Opioids, therefore, are rarely a permanent solution for chronic pain.
As evidenced by the opioid crisis in the United States, non-opioid pain treatments are generally preferred over opioid treatments.
Non-Opioid Pain Medications
Non-opioid pain medications can control mild to moderate pain. Many of these medications are available over-the-counter; however, stronger non-opioid medications are available with a prescription.
In many cases, non-opioid medications, like acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs), are all that are needed to relieve pain.
Non-opioid medications include:
- Non-steroidal anti-inflammatory drugs (NSAIDs) reduce pain, inflammation, and fever.
- Acetaminophen reduces pain and fever, much the same way as NSAIDs, but does not reduce inflammation as well as NSAIDs.
- COX-2 inhibitors are commonly used for arthritis and pain resulting from muscle sprains, strains, back and neck injuries, or menstrual cramps.
- Corticosteroids (“steroids”) are useful in treating both acute and chronic pain by decreasing inflammation, swelling, and pain.
- Topical NSAIDs are often used for osteoarthritis and musculoskeletal pain (like a sprained ankle or pulled muscle). They are applied as gels, creams, sprays, or plasters to unbroken skin.
High-Tech Methods That Help Relieve Chronic Pain
Not all patients of the pain clinic in Lakeland, Florida, with chronic pain will find relief with medications or treatments like physical therapy. For these patients, several “high-tech” treatments may relieve their pain and, in some cases, keep it from coming back. These high-tech methods for reducing chronic pain include:
- Cold laser therapy. This procedure, also called low-level laser therapy, is FDA-approved to treat pain conditions. The cold laser emits pure light of a single wavelength that is absorbed into an injured area and may reduce inflammation and stimulate tissue repair.
- Iontophoresis. This form of electrical stimulation is used to drive medications into areas of pain and reduce inflammation.
- Neurostimulators. This treatment uses implanted electrodes to interrupt nerve signals. This does not cure what is causing the pain but stops the pain signals before they reach the brain. It can be used for back, neck, arm, or leg pain. Trials are currently underway to test their effectiveness on headaches.
- Pain pumps. These devices are implanted in the body and allow the patient to press a button to deliver a dose of pain medication to the area of the spinal cord, often bringing relief without the side effects that often come from oral medications. Patients also receive a psychological boost by having direct control over their pain. Pain pumps are used most often by cancer patients, but also by patients with other types of pain who experience side effects with oral medications.
- Radio waves. Radiofrequency ablation involves inserting a needle next to a nerve and burning it using an electric current created by radio waves. This short-circuits the pain signal from the nerve. Because nerves grow back, the procedure must be repeated; however, relief can be up to a year.
- Injections (nerve blocks). Arthritis, injuries, muscle pain, and headaches are among the kinds of pain treatable with an injection to help short-circuit pain. Using X-ray imagining for guidance, an injection of local anesthetic or other medication blocks or dampens the pain and may stop chronic pain from developing. The location of the injection depends on the source and type of pain. Relief may require a series of injections and repeated treatments.
- Spinal cord stimulation (SCS). Also called neurostimulation, a pacemaker-like device implanted in the lower back replaces pain with a more tolerable sensation, typically a tingling or massage-like feeling from tiny wires placed in the spinal canal. The patient uses a remote control to send signals to the painful area. This technique can help with back pain as well as neuropathy common with diabetes. Newer forms of SCS show promise in relieving pain without the tingling sensation.
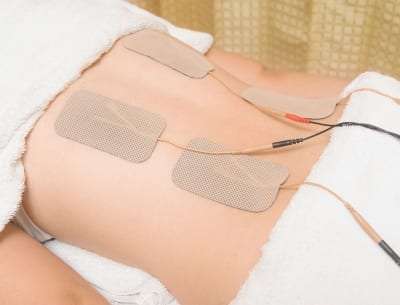
- Transcutaneous electrical nerve stimulation (TENS). This technique employs a very mild electrical current to block pain signals from reaching the brain. Unlike SCS, the stimulator attaches to the skin with small sticky pads connected via wires to a battery-operated device.
- Vein treatments. There are numerous vein conditions that result in pain. Several vein treatments are used to treat these pain conditions including compression therapy, duplex ultrasound, endovenous ablation, phlebectomy, and sclerotherapy.
- Ultrasound. This therapy directs sound waves into tissue. It is sometimes used to improve blood circulation, decrease inflammation, and promote healing.
Alternative Pain Treatments
Some chronic pain sufferers find relief with non-drug therapies that can be used alone or along with non-opioid medications. These treatments include:
- Acupuncture. A technique involving the insertion of extremely fine needles into the skin at specific points on the body to interrupt pain signals. It is believed this action releases endorphins, the body’s natural pain-killing chemicals. It may also influence serotonin levels, the brain transmitter involved with mood.
- Biofeedback. A machine-assisted technique to help patients learn to control their own body responses, including the response to pain.
- Chiropractic. Chiropractors try to correct the body’s alignment to relieve pain, improve function, and help the body heal itself. Chiropractic treatments are often just as effective, if not more, than medication. It is also free of side effects.
- Cold and heat. Cold can be useful immediately after an injury to relieve pain, decrease inflammation and muscle spasms, and help speed recovery. The application of heat raises the patient’s pain threshold and helps relax muscles.
- Exercise. Research shows that staying active is especially important for people with chronic pain. Staying physically active, despite some pain, can play a helpful role for people with some of the more common pain conditions, including low back pain, arthritis, and fibromyalgia. Low-impact exercise helps improve mobility and functionality.
- Massage. For some patients, massage is as effective, if not more effective, than medication. Therapeutic massage may help relieve pain by relaxing painful muscles, tendons, and joints, while also reducing stress and anxiety. Massage is safe and free of side effects.
- Pain-relieving assistive devices. A range of assistive devices can help support painful joints, relieve the pressure on irritated nerves, and soothe aches and pains. Devices include splints, braces, canes, crutches, walkers, and shoe orthotics (inserts).
- Physical therapy (PT) and occupational therapy (OT). PT helps to restore or maintain the ability to move and walk. OT helps improve the ability to perform daily activities such as dressing, bathing, and eating. Both require the patient to attend therapy sessions and do home exercises, which are essential to improving physical healing and relieving pain long term. Whirlpools, ultrasound, and deep-muscle massages may also help.
- Psychotherapy. Specially trained professionals can offer several avenues for pain relief and management that include helping the patient reframe negative thinking patterns about pain. Seeing a mental health professional does not mean the pain is “all in your head.”
- Topical pain relievers. These are medication-containing creams, ointments, and patches that are applied to the skin. They may be used in place of, or in addition to, other pain treatments for osteoarthritis and musculoskeletal pain.
- Weight loss. Many painful health conditions are worsened by excess weight. Losing weight can help relieve certain types of pain.
- Yoga and tai chi. These mind-body exercises incorporate breath control, meditation, and movements to stretch and strengthen muscles. They may help with chronic pain conditions such as fibromyalgia, low back pain, arthritis, and headaches.
Among the millions of chronic pain sufferers in the nation, no two cases are the same. Everyone is unique, and what works for one patient may not work for another. When other treatments aren’t effective, surgery may be an option to correct an abnormality that is responsible for the pain.
While there may not be a cure for your chronic pain, many pain treatments are available to help you effectively function. It is essential, therefore, to work closely with your pain doctor to find the best solution for pain management.
Novus Spine & Pain Center
Novus Spine & Pain Center is in Lakeland, Florida, and specializes in treating chronic pain with non-opioid pain treatments. By using a comprehensive approach and cutting-edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
Our Mission Statement: To provide the best quality of life to people suffering from pain, by providing state of the art treatments, knowledge and skill, compassion, and respect for all.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Non-Opioid Medications Resources
Non-Opioid Treatment (American Society of Anesthesiologists)
Non-opioid options for managing chronic pain (Harvard Health)
Non-pharmacologic and non-opioid solutions for pain management (Joint Commission)
Chronic Pain Management (PubMed)
Updated: January 31, 2022

