 In the past, the only effective way to treat bulging, twisting varicose veins was to remove them through surgery. The procedure, known as vein stripping, involved significant discomfort and downtime, discouraging many from seeking treatment. Fortunately, traditional surgical procedures have given way to less invasive methods in the treatment of varicose veins and their pain management today. One of these techniques, used at the vein clinic at Novus Spine & Pain, is phlebectomy.
In the past, the only effective way to treat bulging, twisting varicose veins was to remove them through surgery. The procedure, known as vein stripping, involved significant discomfort and downtime, discouraging many from seeking treatment. Fortunately, traditional surgical procedures have given way to less invasive methods in the treatment of varicose veins and their pain management today. One of these techniques, used at the vein clinic at Novus Spine & Pain, is phlebectomy.
Phlebectomy is one of the oldest forms of treatment for varicose veins; the earliest description of it was written by Aulus Cornelius Celsus, a Roman historian of medicine, in 45 AD. The modern technique of ambulatory (outpatient) phlebectomy was developed around 1956 by Swiss dermatologist, Robert Muller.
In This Article:
- What Is Phlebectomy?
- The Problem with Vein Stripping
- The Phlebectomy Procedure
- What is the difference Between Phlebectomy and EVLT?
- Advantages of Phlebectomy
- How Well Does Phlebectomy Work?
- Novus Spine & Pain Center
- Phlebectomy Resources
What Is Phlebectomy?
Phlebectomy is a minimally invasive procedure that uses a small scalpel or needle to remove varicose veins that lie just beneath the surface of the skin. Also called Ambulatory Phlebectomy, Microphlebectomy, and Stab Avulsion, the procedure consists of several tiny cuts (also called “stab incisions”) in the skin through which the varicose vein is removed piece by piece. The incisions are generally so small that stitches are not required.
Performed in the physician’s office, using local anesthesia, the procedure allows the doctor to remove an affected vein in small sections through smaller openings than vein stripping requires. Phlebectomy is a safe and effective treatment for removing small to medium varicose veins. It is rare to remove spider veins by this method.
The procedure involves minimal discomfort and downtime and the patient can get up and walk following the procedure. Typically, a patient can resume a normal daily routine the next day. The doctor will likely have the patient wear a compression bandage or compression stocking for at least a week to help the healing process. The procedure may produce some temporary swelling and bruising.
Most patients will not require any prescription pain medicine following treatment. Most discomfort can be sufficiently managed through ice packs and over-the-counter medication. Downtime is also minimal, with most patients returning to work and regular activities the day after the procedure.
Often, phlebectomy is used in conjunction with other common vein removal procedures such as endovenous laser therapy (EVLT) and sclerotherapy to address differently sized veins and to yield the best cosmetic results.
The Problem with Vein Stripping
Vein ligation and vein stripping are the surgical approaches treating varicose veins. Ligation refers to surgically tying off the greater saphenous vein (the large vein running from the ankle to the groin) in the leg while vein stripping is the removal of the vein.
Both of these procedures require a large incision in the groin area or behind the knee to access the vein.
Vein ligation and stripping are invasive procedures that tie off the varicose vein and pull it out of the body through the incisions in the groin and ankles. Today, physicians realize removal of the greater saphenous vein is no longer necessary. Vein stripping is rarely performed today because newer, less invasive options like endovenous thermal ablation are considered superior treatment in most cases.
In fact, many physicians no longer recommend ligation and stripping because there is a fairly high recurrence of varicose veins after the procedure. Ligation also has severe side effects, including potential numbness around the treated area. In rare cases, patients can experience blood clots, scarring, infections, and even severe pain.
The Phlebectomy Procedure
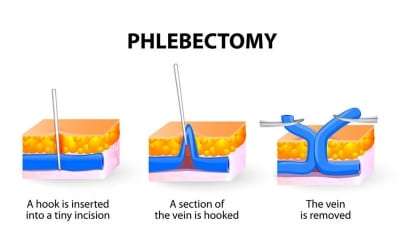
After identifying which veins will be removed, the doctor marks the areas where incisions will be made. A local anesthesia is administered at various points along the vein to be removed. Once the anesthesia has taken effect, the doctor makes a few tiny incisions cutting the vein into sections. A tiny hook gently removes the sections of the vein. Removing the vein in sections minimizes the occurrence of blood clots, and encourages faster healing.
Once the procedure is complete, a dressing is applied over the incisions. An elastic compression dressing is applied from the foot up the leg to cover the incisions. In some cases, compression stockings will be worn. The patient is encouraged to walk around for 10–15 minutes before leaving the office. This mild activity helps minimize the risk of a blood clot forming in the deep veins of the leg.
The bandages may be removed a few days after the procedure. The compression stockings must be worn for a couple of weeks to minimize bruising and swelling.
Bed rest is generally prohibited after venous surgery. Instead, daily walking and movement are greatly encouraged following a phlebectomy.
What Is the Difference Between Phlebectomy and EVLT?
Endovenous Laser Treatment (EVLT) uses lasers to treat larger varicose veins and problem veins which are deep under the skin. EVLT is often performed first to remove larger varicose veins which are often the source of vein problems.
Following EVLT treatment, a doctor may also perform a phlebectomy to remove smaller or more surface veins that remain. A combination of EVLT and phlebectomy can often be used to remove problem veins for a better cosmetic result.
Advantages of Phlebectomy
When performed by a skilled physician, research shows that phlebectomy yields a long-term success rate of 90%. Once initial bruising resolves there is a noticeable reduction in varicose veins. In addition, a phlebectomy has the following benefits over other procedures:
- Phlebectomy is minimally invasive.
- The procedure only requires local anesthesia.
- Phlebectomy may be used in combination with other procedures like EVLT and sclerotherapy.
- Recovery time is quick, with an almost immediate return to normal daily activities.
- About 95% of phlebectomy patients experience significant relief of pain.
How Well Does Phlebectomy Work?
Long-term results following a phlebectomy are excellent when the procedure is performed for the appropriate conditions. Although phlebectomy can help improve the cosmetic appearance of the skin, the procedure is less likely to fix varicose veins when the leg veins are not working well. Often the procedure is done in conjunction with other treatments. Depending on the patient, laser treatment or radiofrequency treatment may be used. In some cases, ligation and stripping are required.
A phlebectomy is not recommended for patients who are unable to walk on their own or cannot wear compression stockings.
Novus Spine & Pain Center
Novus Spine & Pain Center is in Lakeland, Florida, and treats patients with chronic pain with numerous therapies including phlebectomy. By using a comprehensive approach and cutting-edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Phlebectomy Resources
Varicose Veins: Phlebectomy or Stab Avulsion (University of Wisconsin-Madison Health)
Ambulatory Phlebectomy (American Society for Dermatologic Surgery)
Microphlebectomy (Vein Directory)
Medical Definition of Phlebotomy (MedicineNet)
Ambulatory phlebectomy (Wikipedia)
Vein Stripping (Wikipedia)
Varicose Vein Surgery (Vein Directory)
Vein Ligation and Stripping (Encyclopedia of Surgery)
Ambulatory phlebectomy versus compression sclerotherapy: results of a randomized controlled trial (PubMed)
Ambulatory Phlebectomy for Varicose Veins – Outcomes (Medscape)
Updated: July 9, 2021

