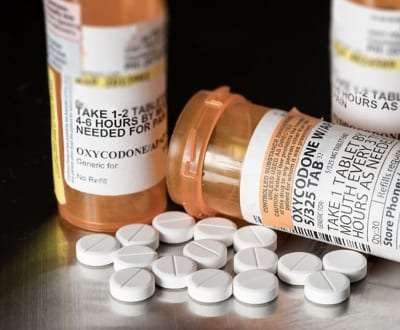
 Opioid addiction is a growing problem in America. The Government estimates 90 percent of Americans struggling with opioid addiction are not getting treatment. To fight opioid addiction, pain management strategies are implemented to lessen or eliminate the need for opioids and avoid opioid addiction.
Opioid addiction is a growing problem in America. The Government estimates 90 percent of Americans struggling with opioid addiction are not getting treatment. To fight opioid addiction, pain management strategies are implemented to lessen or eliminate the need for opioids and avoid opioid addiction.
Furthermore, the U.S. Department of Health and Human Services is providing $485 million in grants to help combat opioid addiction. The funding is the first of two rounds being issued to all 50 states to support a comprehensive array of prevention, treatment, and recovery services. Beyond this initial grant, another half-billion-dollar grant will be released to states.
The Federal Government wants to combat this growing health emergency by improving access to treatment and recovery services. By providing cutting-edge research on pain and addiction, as well as better pain management practices, it is hoped the opioid addiction can be reduced.
In This Article:
- The Opioid Addiction Crisis
- What Are Opioids?
- Why are Opioids So Addictive?
- Pain Management Strategies to Avoid Opioid Addiction
- Lakeland Pain Management Experts
- Novus Spine & Pain Center
- Opioid Addiction Resources
The Opioid Addiction Crisis
In 2015, 52,000 people died of overdoses in America, with a majority of the deaths related to opioids.
It is estimated that 140 Americans die every day from an opioid overdose, with the most deaths occurring in southern states. Most troubling, however, is that nearly half of all U.S. opioid overdose deaths involve a prescription opioid.
Opioids like fentanyl can be very lethal and are easily obtainable today. Fentanyl is a powerful synthetic opioid similar to morphine, but 50 to 100 times more potent. It is typically used to treat patients with severe pain or to manage pain after surgery. It is also used to treat chronic pain in some patients. Fentanyl also delivers a feeling of euphoria as it deadens pain, making it a popular street drug. It is highly addictive and so powerful that it can kill with just one dose.
Prescription drug misuse has serious medical consequences. Increases in prescription drug abuse over the last 15 years are reflected in increased emergency room visits, overdose deaths associated with prescription drugs, and treatment admissions for prescription drug use disorders. The most severe form is addiction. As a result, unintentional overdose deaths involving opioid pain relievers have more than quadrupled since 1999, and have outnumbered those involving heroin and cocaine since 2002.
What Are Opioids?
Opiates are drugs derived from opium. At one time, the word “opioids” referred to synthetic opiates only, but now the term is used for the entire family of opiates (natural, synthetic, and semi-synthetic).
Opioids work by attaching to receptors (a part of the cells) found in the brain, spinal cord, and other areas of the body. They help blunt the intensity of pain signals reaching the brain, which reduces the sensation of pain and discomfort. Therefore, taking an opioid raises the pain threshold in the body. Instead of pain, the brain senses feelings of pleasure from the release of artificial endorphins.
Opioid pain medication is commonly used to lessen pain following surgery, after a severe injury, and to relieve chronic pain. Milder forms of opioids are often prescribed to help suppress coughs or ease severe diarrhea.
There are many ways to take opioid medications:
- Pill or liquid by mouth.
- Nasal spray.
- Skin patch.
- Tablet dissolved under the tongue or between the gum and cheek.
- Suppository.
- Injection into a vein, muscle, or around the spinal cord.
- Implanted pump.
The administration of an opioid depends on the specific situation. Generally, opioids are prescribed for pain that lasts only a few days because of their addictive nature. Doctors are likely to use them:
- When there is a flare up of severe pain.
- When other treatments fail to work.
- To help control pain while waiting for other treatments to take effect.
Why Are Opioids So Addictive?
Opioids act on the brain to trigger the same processes that provide feelings of pleasure from activities we enjoy (for instance eating), but they do it far more intensely. Opiates do this by creating artificial endorphins in the brain. Some opioids create over 100 times more endorphins than the body would naturally produce.
The artificial production of endorphins causes the body to stop producing them naturally. When the body stops producing its own endorphins, the person may feel sick and depressed. The only way to compensate for the lost endorphins is to take more and more of the drug, which makes opioids so addictive.
After continued use of opioids, the desire is no longer about positive feelings. Instead, the addiction comes from a desire to avoid the negative feeling and symptoms the user now encounters. When this “switch” occurs (i.e., achieving good feelings turns to avoiding bad feelings), the person has become addicted to opioids. Opioids can also impair self-control if taken long enough, making it harder to stop using them, even if the drug no longer provides pleasure and the user wants to stop.
When people addicted to opioids stop taking the drug, they experience withdrawal. The symptoms can occur almost immediately. Withdrawal symptoms can include stress, anxiety, suicidal thoughts, depression, restlessness, lack of sleep and other debilitating effects.
Addiction happens in about 5% of people who take opioid pain relievers as directed for a period of one year. Opioids can provide much-needed relief, but there are risks and side effects. If an opioid is prescribed, it is important to stay in touch with the prescribing physician while taking the medication to avoid addiction.
Pain Management Strategies to Avoid Opioid Addiction
Pain is real, and it’s physical. Proper and efficient pain management requires approaching pain from both the physical and emotional levels. We all have a different threshold for pain and tolerance for pain. Today, pain management strategies include a combination of noninvasive therapies. A partial list of the various treatments includes:
Non-Opioid Medications
Unfortunately, no single drug works for everyone, and not everyone benefits from prescription drugs.
- Anticonvulsants. Medications that work by quieting damaged nerves to slow or prevent uncontrolled pain signals.
- Antidepressants. Medications that work by modifying the chemical messengers that relay pain signals. Antidepressants may also help with sleep, which can help patients feel better.
- Anti-inflammatories. Nonsteroidal anti-inflammatory drugs (NSAIDs) relieve pain and curb inflammation.
- Muscle Relaxants. Medications that can calm muscle spasms that cause pain.
- Steroids. Medications that help alleviate inflammation and pain.
Noninvasive Therapies
As with medications, noninvasive treatment techniques are a matter of trial and observation. The following techniques are just a few of those available to help relieve pain. Consult your doctor before beginning any treatment, even if it is noninvasive.
- Acupuncture. Studies by the National Institutes of Health show that acupuncture can be an effective treatment for some types of chronic pain. Acupuncture includes a practitioner inserting extremely fine, sterilized stainless-steel needles into the skin at specific points on the body.
- Biofeedback. The process of biofeedback makes patients more aware of typically automatic processes inside the body (such as muscle tension, temperature, and heart rate). Biofeedback helps the patient gain some conscious control of these processes. This awareness of the body helps with relaxation, which can help relieve the pain.
- Chiropractic manipulations are targeted adjustments and manipulations that can help correct certain pain signal transmissions.
- Cognitive-behavioral therapy is a type of psychotherapy that helps the patient understand what pain means, and develop skills to change negative thoughts about their pain. By changing negative thoughts and behaviors, people can change their awareness of pain and develop better skills for coping, even if the actual level of pain stays the same.
- Heat application. Sometimes the application of heat can ease the pain.
- Massage. Focused rubbing of the affected area may contribute to relieving the discomfort associated with pain. Massage can also help the patient relax, decreasing stress and tension.
- Meditation. A practice that soothes the brain patterns underlying pain, and eventually alters the structure of the brain itself, so the patient no longer feels pain with the same intensity.
- Physical therapy. Once acute pain is under control, a physical therapist may design a rehabilitation program to help prevent future injuries. Typical physical therapy involves exercises intended to strengthen muscles and improve flexibility.
- Relaxation techniques include various methods that help the mind alter its focus to something other than the source of pain.
- Transcutaneous Electrical Nerve Stimulation (TENS) is a device that sends a weak electrical current via adhesive patches with small electrodes attached to the skin near the area of pain. The stimulation may interrupt or mask pain signals, preventing them from reaching the brain.
- Yoga. The benefits of stretching and yoga can help alleviate pain, depending on the cause of the pain.
Minimally Invasive Therapies
- Cryotherapy. Electrical stimulation from a probe helps identify affected nerves. Once identified, freezing cycles are initiated over the painful nerves.
- Injection. Sometimes pain-killing medication, such as local anesthetics and steroids, can provide pain relief.
- Nerve block, which is an anesthetic or anti-inflammatory injection that helps interrupt pain messages between the brain and the site of the pain.
- Spinal Cord Stimulation (SCS). A neurostimulator delivers mild electrical impulses to the epidural space near the source of chronic pain. The pulses interfere with pain signals to the brain. A trial stimulator is typically worn for five to seven days externally. If the trial successfully relieves the pain, the patient may decide to have a permanent SCS placed under the skin.
Surgery
Surgery may be an option when more conservative measures do not succeed. Surgery is typically used to reduce pressure on certain nerves, which helps alleviate chronic pain.
Lakeland Pain Management Experts
Dr. Benito Torres is a pain management doctor in Lakeland, Florida, specializing in the pain management of conditions such as acute headaches, arthritis, back pain, cancer pain, carpal tunnel syndrome, sciatica, scoliosis, shingles, whiplash, and much more.
Dr. Torres completed his residency in Physical Medicine and Rehabilitation at the University of Toledo, followed by an ACGME accredited 2-year Pain Medicine Fellowship at the University of South Florida. Dr. Torres is Board certified in Physical Medicine and Rehabilitation and Pain Medicine through the American Board of Physical Medicine and Rehabilitation. Following completion of his training, Dr. Torres accepted a position as faculty in the Department of Anesthesia at Moffitt Cancer Center, providing pain relief through minimally invasive procedures.
Today, Dr. Torres continues to hold a Clinical Assistant Professor appointment in the Department of Physical Medicine and Rehabilitation at the University of South Florida and Department of Neurology, teaching Residents and Pain Medicine Fellows.
Novus Spine & Pain Center
Dr. Torres established Novus Spine & Pain Center in Lakeland, Florida with a goal of providing the highest quality pain management care to every patient. Whether pain is the result of an injury or from another condition, Dr. Torres offers many different treatment options.
Novus Spine & Pain Center utilizes a comprehensive approach and cutting-edge therapies to restore normal function and allow patients to regain an active lifestyle while minimizing the need for opiates. As our patient, you are our top priority. Our goal is to help you achieve the best possible quality of life.
Our Mission Statement: To provide the best quality of life to people suffering from pain, by providing state of the art treatments, knowledge and skill, compassion, and respect for all.
To schedule an appointment, please contact us online, request a call back, or call our office at 863-583-4445.
Opioid Addiction Resources
Secretary Price Announces HHS Strategy for Fighting Opioid Crisis (U.S. Department of Health & Human Services)
Trump Administration Awards Grants to States to Combat Opioid Crisis (U.S. Department of Health & Human Services)
Fentanyl (NIH – National Institue on Drug Abuse)
Misuse of Prescription Drugs (NIH – National Institue on Drug Abuse)
What Are Opioids? (WebMD)
Prescription Opioid Overdose Data (Centers for Disease Control and Prevention)
Manage Opioids (WebMD)
The Neurobiology of Opioid Dependence: Implications for Treatment (PubMed)
Science Says: Why are opioids so addictive? (AP News)
Why Are Opiates So Addictive? (Michael’s House)

