 Dorsal root ganglion (DRG) stimulation is a pain management option for people with difficult-to-treat chronic pain in specific areas of the lower body, such as the foot, knee, hip, or groin. It is similar to spinal cord stimulation (SCS), which can block pain signals from a large area of the body; however, DRG targets more specific areas of the body.
Dorsal root ganglion (DRG) stimulation is a pain management option for people with difficult-to-treat chronic pain in specific areas of the lower body, such as the foot, knee, hip, or groin. It is similar to spinal cord stimulation (SCS), which can block pain signals from a large area of the body; however, DRG targets more specific areas of the body.
In This Article:
- What is a Dorsal Root Ganglion?
- What is Dorsal Root Ganglion Stimulation?
- Conditions Treated with Dorsal Root Ganglion
- How Does Dorsal Root Ganglion Work?
- Who Can Benefit from Dorsal Root Ganglion?
- Novus Spine & Pain Center
- Dorsal Root Ganglion Resources
What is a Dorsal Root Ganglion?
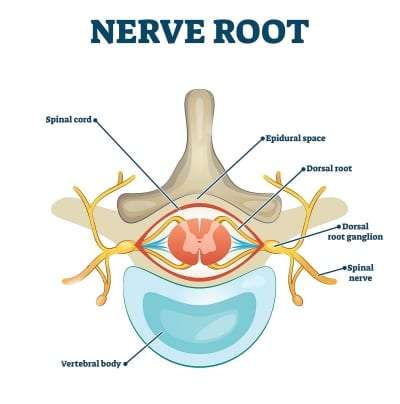
A ganglion is a part of the peripheral nervous system that connects the central nervous system to the organs, limbs, and skin. One of the types of ganglia present in the peripheral nervous system is a dorsal root ganglion.
The dorsal root ganglion (DRG) is a part of the spine where nerves branch off from the dorsal column (the back of the spinal cord). These branches of nerves then spread throughout the body. The DRG relays both pain and non-pain signals from the body to the central nervous system.
What Is Dorsal Root Ganglion Stimulation?
Dorsal root ganglia stimulation can be beneficial in the management of chronic pain. The pain management system consists of electrical leads and an implantable pulse generator. The electrical leads have contacts that are placed over the DRG near the spinal cord. Although similar to spinal cord stimulation, DRG stimulation is more selective in targeting painful areas that can be difficult to reach with SCS.
A small pulse generator is implanted in the upper buttock/low back or, with an extension, into the abdominal wall. Patients have a small handheld controller that can change the stimulation settings.
Conditions Treated with Dorsal Root Ganglion Stimulation
In February 2016, the U.S. Food and Drug Administration approved dorsal root ganglion stimulation for patients with Complex Regional Pain Syndrome (CRPS Type 1 and 2) in the lower extremities. The procedure is similar to traditional spinal cord stimulation (SCS).
This kind of stimulation is better for smaller, more specific areas of pain because it can target a more specific location than traditional SCS. It is particularly effective in relieving chronic lower limb pain associated with complex regional pain syndrome (CRPS) and peripheral causalgia (nerve damage).
How Does Dorsal Root Ganglion Stimulation Work?
DRG stimulation therapy works by stimulating dorsal root ganglia. These nerve bundles regulate the sensations that travel through nerve fibers along the spinal column to the brain. Each bundle is associated with different areas of the body. DRG stimulation therapy targets DRGs associated with the specific area of the body where a patient experiences pain.
The DRG stimulation consists of three parts that work together to help manage pain:
- Generator. A small electronic device implanted in the body that generates mild electrical pulses.
- Leads. Thin insulated wires that carry the electrical pulses from the generator to the dorsal root ganglia. The leads are placed over the DRG.
- Patient controller. A handheld “remote control” that allows the patient to adjust the strength and location of stimulation.
Implanting the DRG stimulator is similar to having an SCS device implanted. The process begins with a trial that typically lasts 5 to 7 days. The trial stimulator leads are temporarily implanted through the skin into the epidural space (the area surrounding the spinal cord). Once in place, the leads are connected to a trial stimulator worn outside the body on a belt.
When activated, the leads send tiny electrical impulses to the dorsal root ganglion. The impulse blocks pain signals to the brain. During the trial, the patient can control the device to alleviate pain. The patient can turn the device on and off as needed and adjust the amount of stimulation.
After the trial, the patient and physician determine if a permanent device would be helpful. For permanent implantation, the DRG stimulator’s electrical pulses are programmed with an external control remote unit that the patient uses to control the system.
There are four distinct advantages of targeting the dorsal root ganglion for pain relief:
- Directed anatomical targeting. DRG stimulation offers a highly-directed stimulation field, which can limit stimulation to the targeted area. A clinical trial of DRG stimulation for chronic lower limb pain found that 94.5 percent of the patients reported no extraneous sensations outside the targeted area. Only 61.2 percent of patients in the SCS control group reported similar results.
- Low energy requirements. The dorsal root ganglion is surrounded by a thin layer of spinal fluid, which requires less energy than is needed for traditional SCS and leads to longer battery life.
- A marginal risk of lead migration. The dorsal root ganglion is in a very confined space, which reduces the chances of leads moving. Traditional SCS reports a 14 percent lead migration rate.
- Minimal postural effects. The dorsal root ganglion is located in a small space that does not vary with body position. The patient receives the same stimulation – and pain relief – whether lying, standing, sitting, or walking. With traditional SCS therapy, a change in the patient’s posture can cause a difference in intensity or an abnormal tingling or pricking sensation. DRG provides a more focused stimulation that is typically confined to the painful area while helping to avoid unwanted stimulation.
In one survey of over 200 patients with a permanent DRG stimulator implant, the patients reported substantial pain improvement. The survey found DRG stimulation to be an effective and safe therapy for chronic pain.
Who Can Benefit from DRG Stimulation?
Traditional spinal cord stimulation has been utilized since 1967, and although the technology has evolved, it is not a remedy for all chronic pain patients. Studies show that about half of the patients report satisfactory relief with their SCS implant.
The FDA has approved DRG stimulation for lower extremity CRPS, which could include neuropathic pain conditions and chronic pain following foot, knee, groin, and other surgeries. Doctors believe one of the best future indications for DRG stimulation is diabetic neuropathy. Over time, high blood sugar levels tend to damage the peripheral nerves in the legs and feet. Neuropathic pain is often managed with medication, which can cause side effects. DRG stimulation can target both feet and help relieve the diabetic neuropathy pain without medication and any associated side effects.
DRG stimulation therapy may be an option for patients with chronic pain that has lasted six months or more and have found little or no relief from traditional neurostimulation, surgery, pain medications, nerve blocks, or other pain management therapies. If you suffer from this kind of pain, DRG stimulation may work where other therapies have not been effective.
Novus Spine & Pain Center
Novus Spine & Pain Center is in Lakeland, Florida, and treats patients with chronic pain with numerous therapies, including dorsal root ganglion stimulation. By using a comprehensive approach and cutting edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Dorsal Root Ganglion Resources
Neuroanatomy, Dorsal Root Ganglion (PubMed)
Dorsal Root Ganglion (Neuroscientifically Challenged)
Dorsal Root Ganglion (Brain Made Simple)
Dorsal Root Ganglion Stimulation (International Neuromodulation Society)
Dorsal Root Ganglion Stimulation Offered for CRPS in Lower Extremities (Cleveland Clinic)
Dorsal Root Ganglion Stimulation Therapy (Penn State Health)
Effectiveness and Safety of Dorsal Root Ganglion Stimulation for the Treatment of Chronic Pain: A Pooled Analysis (PubMed)
Updated: 9/23/22

