 Spinal cord stimulation (SCS) is a cutting-edge technology that addresses some of the most difficult chronic pain problems experienced today. It can improve the overall quality of life and reduce the need for pain medicines. SCS may also be used with other pain management treatments.
Spinal cord stimulation (SCS) is a cutting-edge technology that addresses some of the most difficult chronic pain problems experienced today. It can improve the overall quality of life and reduce the need for pain medicines. SCS may also be used with other pain management treatments.
Spinal cord stimulation has been used for decades. First used to treat pain in 1967, the Food and Drug Administration (FDA) approved spinal cord stimulation in 1989 for the relief of nerve damage in the trunk, arms, or legs. The procedure now accounts for about 90 percent of all neuromodulation treatments (the alteration of nerve activity through targeted delivery of a stimulus, such as electrical or chemical agents). According to the International Neuromodulation Society, about 34,000 patients undergo spinal cord stimulator implants each year around the world.
In This Article:
- What is a Spinal Cord Stimulator Implant?
- Conditions Treated with Spinal Cord Stimulation
- Types of Spinal Cord Stimulator Implants
- What are the Advantages of Spinal Cord Stimulation?
- Who Can Benefit from a Spinal Cord Stimulation
- Living with a Spinal Cord Stimulator
- Novus Spine & Pain Center
- Spinal Cord Stimulator Implant Resources
What is a Spinal Cord Stimulator Implant?
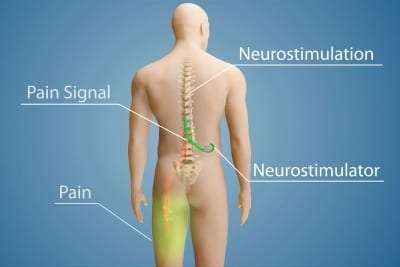
A spinal cord stimulator is an implanted device that directs mild (low level) electrical pulses along implanted wires to an area near the spinal cord. The source of the pulse is a small device implanted near the spine. The technique is also called neurostimulation. The stimulator is similar to a cardiac pacemaker, leading some to call the device a “pacemaker for pain.”
The pulse from the stimulator interrupts the perception of pain, substituting it with a more pleasing sensation (paresthesia). The feeling differs from patient to patient, but most describe it as a mild or pleasant tingling. The patient experiences a reduction in pain because the stimulator’s electrical pulse interrupts the transmission of pain signals to the brain.
Careful screening is needed because spinal cord stimulation does not work for everyone. For those who are good candidates, most report at least a 50% reduction in pain, as well as a significant improvement in daily function.
If the person fits the criteria for spinal cord stimulation, the doctor will arrange a trial period to see how well the temporary therapy eases the individual’s pain. Unlike many other treatments, a spinal cord stimulator can be used for a short, trial period before the patient commits to having the implant.
The trial procedure typically requires only one incision to place flexible wires (electrodes) near the spine. The wires are connected to an external stimulator that is carried outside the body, typically on a belt.
The trial period can last up to 10 days, during which time the patient evaluates how well the device reduces pain. The trial is considered a success if there is a 50% or greater reduction in pain.
If unsuccessful, the wires can easily be removed in the clinic without damage to the spinal cord or nerves. If successful, surgery is scheduled to implant the stimulator under the skin. The generator is usually placed in the abdomen, upper buttocks, or upper chest.
Conditions Treated with Spinal Cord Stimulation
Spinal cord stimulation is recommended for an increasing number of painful conditions. It is most often used after nonsurgical pain treatment options have failed to provide sufficient relief. Spinal cord stimulators are used to treat or manage different types of chronic pain, including:
- Arachnoiditis, a painful inflammation of the arachnoid, a thin membrane that covers the brain and spinal cord.
- Back pain, especially back pain that continues after surgery (failed back surgery syndrome).
- Chronic neck pain that can include arm pain.
- Complex regional pain syndrome (CRPS), a chronic, progressive disease characterized by severe pain and swelling.
- Heart pain (angina) that is untreatable by other means.
- Injuries to the spinal cord from a fall, an accident, sports injury, and similar traumatic injuries.
- Nerve-related pain such as severe diabetic neuropathy and cancer-related neuropathy from radiation, surgery, or chemotherapy.
- Phantom limb pain following an amputation.
- Peripheral neuropathy, a constant burning pain of the legs.
- Peripheral vascular disease caused by an arm or leg injury, infection, or irregular muscle or ligament anatomy.
- Post-surgical pain, chronic pain that lasts more than three months after surgery.
- Refractory angina, which causes chest pain, shortness of breath, and fatigue.
Patients who continue to experience pain after one or more back (or neck) surgeries that fail to alleviate persistent low back pain, leg pain (sciatica or lumbar radiculopathy), or arm pain (cervical radiculopathy) are also good candidates for a spinal cord stimulator implant.
Spinal cord stimulation can improve the overall quality of life and sleep while reducing the need for pain medicines. It is typically used along with other pain management treatments, including medications, exercise, physical therapy, and relaxation methods.
Types of Spinal Cord Stimulator Implants
There are three main types of spinal cord stimulators:
- Conventional implantable pulse generator (IPG). This stimulator is a battery-operated unit that is placed in the spine during an operation. Battery replacement requires another surgery. This device can be a good choice for people with pain in just one body part because it has a lower electrical output.
- Rechargeable IPG. This stimulator is similar to the conventional device, except the battery can be recharged without the need for additional surgery. Because the energy source is rechargeable, these stimulators can produce a higher electrical output. This type of unit may be a better choice for people with pain in the lower back, or one or both legs because the electrical signal travels farther.
- Radiofrequency stimulator. This stimulator is rarely used today because of newer designs and better technology. It has rechargeable batteries that are outside the body. Like the rechargeable IPGs, it may be better for people with pain in the lower back and legs because of the device’s power.
All three devices allow for the adjustment of the intensity of the electrical signal. Different body positions may require different stimulator settings, such as a setting for sitting and another for walking. Most devices have preset programs with different settings.
What are the Advantages of Spinal Cord Stimulation?
Finding effective treatment for chronic pain, especially chronic back, and neck pain can be challenging.
A review of spinal cord stimulation systems for chronic pain finds that spinal cord stimulation is potentially effective for many chronic pain conditions that have not been helped by other treatments.
Spinal cord stimulator implant treatment has several advantages over many surgical procedures:
- Spinal cord stimulation therapy is reversible. If the patient decides to discontinue the therapy at any time, the electrical contacts, wires, and generator can be removed without any permanent changes to the spine.
- Adjustable pain relief. Pain varies widely from person to person and can vary within an individual at different times. Most stimulators allow the patient to adjust their device. Some models adjust automatically to the person’s movements.
- Minimally invasive procedure. Only one incision is necessary to implant the generator. The placement of the electrodes is done by either making an incision or using a hollow needle.
- Reduced opioid use. The pain relief experienced with spinal cord stimulation allows many patients to take fewer pain medications. Research finds that more than a third of participants in one study receiving high-frequency therapy reduced or stopped taking opioid medications.
- Targeted pain relief. Instead of taking a medication that affects the whole body and causes unrelated side effects (sleepiness, constipation, etc.), spinal cord stimulation delivers pain relief only where it is needed.
- Limited or no side effects. The therapy does not have the type of side effects associated with many other treatments, including medications.
- Alternative to oral medication. The therapy is an effective pain control option for those who have problems taking oral medication.
- No refills are necessary. Spinal cord stimulation pain relief can continue for years, without prescription refills or frequent office visits.
Who Can Benefit from a Spinal Cord Stimulation?
The Lakeland, Florida Pain Doctor recommends spinal cord stimulation when other treatments have not been successful, when surgery is not likely to help, or when surgery has failed. It can also be an option for treating chronic pain associated with sciatica, failed back surgery or nerve pain, or for people who have not benefitted from more conservative therapies.
While the degree of pain relief varies from person to person, many also report a significant increase in their ability to again enjoy normal family and work activities. In addition, reducing pain can have a positive effect on mental outlook and improve the patient’s overall quality of life.
Living with a Spinal Cord Stimulator
Generally, the pain relief provided by spinal cord stimulators allow patients to do much more than they could previously, but there are certain restrictions:
- X-rays and CT scans. As long the spinal cord stimulator is powered off, X-rays and CT scans are generally safe. Before undergoing any scan, always let your doctor, nurse, or technician know you have a spinal cord stimulator.
- MRI scans. MRIs are not always safe with a spinal cord stimulator, depending on several factors. Some newer devices are compatible with specific MRI machine models and scan locations. Still, it is necessary to speak with your doctor. If a device is not MRI compatible, MRIs can cause serious injury.
- Airport security gates will detect a stimulator. However, spinal cord stimulator patients can carry an identification card that may allow bypassing the machine. Some people report airport security gates cause uncomfortable (but harmless) interference with their stimulators. If you cannot avoid the security, turn off your device before stepping through the security screener.
- Driving. Always power off the stimulator when driving or operating heavy machinery, as sudden changes in stimulation levels could cause a distraction.
- Swimming is okay with a permanent, implanted generator, but you cannot get a temporary stimulator wet. The patient will need to avoid baths and showers during the trial period.
It is important to point out that spinal cord stimulator implant treatment is not for all pain patients. It is usually not recommended for individuals who:
- Have a systemic infection (entire body) or an infection at the site where the device would be implanted.
- Use a demand-type cardiac pacemaker.
- Have severe depression or another psychiatric condition that could be contributing to the pain.
- Have untreated bleeding disorders.
- Have untreated drug addiction issues.
Doctors typically advise smokers to quit before beginning spinal cord therapy, because tobacco is linked to worse outcomes with the devices. Recreational drug use is also thought to reduce the chance of successful treatment with a spinal stimulator.
Nationwide, pain management doctors are using pain-relief treatments that do not involve medications, including spinal cord stimulation, to reduce reliance on opioid pain medications.
If you suffer from chronic pain, and other forms of pain management have not successfully controlled your pain, a spinal cord stimulator may be an appropriate option to help improve your life.
Novus Spine & Pain Center
Novus Spine & Pain Center is in Lakeland, Florida, and treats patients with chronic pain with numerous therapies, including spinal cord stimulator implants. By using a comprehensive approach and cutting edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Spinal Cord Stimulator Implant Resources
Spinal Cord Stimulator (Johns Hopkins)
Spinal Cord Stimulation (American Association of Neurological Surgeons)
Incidence and predictive factors of spinal cord stimulation treatment after lumbar spine surgery (PubMed)
How it Works: SCS Spinal Cord Stimulation (Medtronic)
Back Pain and Spinal Cord Stimulation (WebMD)
Spinal Cord Stimulation for Chronic Back and Neck Pain (Spine-Health)
Who May Benefit from Spinal Cord Stimulation (Spine-Health)
Spinal Cord Stimulation Procedure (Spine-Health)
Advantages of Spinal Cord Stimulation (Spine-Health)
Spinal Cord Stimulation (Virginia Spine Institute)
Spinal Cord Stimulation Implant (University of Pittsburgh Medical Center)
A review of spinal cord stimulation systems for chronic pain (PubMed)
Novel 10-kHz High-frequency Therapy (HF10 Therapy) Is Superior to Traditional Low-frequency Spinal Cord Stimulation for the Treatment of Chronic Back and Leg Pain (American Society of Anesthesiologists)
Neuromodulation (medicine) (Wikipedia)
Updated: May 18, 2022

