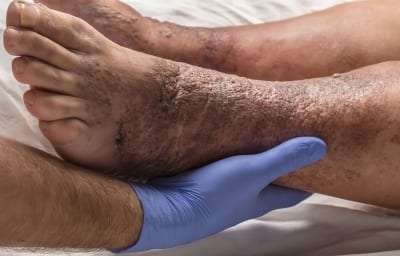
 Stasis dermatitis is a common inflammatory skin disease that occurs in the lower extremities. Although not as prevalent as skin cancer, stasis dermatitis affects a significant proportion of the elderly in the United States. Slightly more women than men have stasis dermatitis, which afflicts approximately 20 percent of people over the age of 70. Furthermore, stasis dermatitis is more prevalent among people who are overweight.
Stasis dermatitis is a common inflammatory skin disease that occurs in the lower extremities. Although not as prevalent as skin cancer, stasis dermatitis affects a significant proportion of the elderly in the United States. Slightly more women than men have stasis dermatitis, which afflicts approximately 20 percent of people over the age of 70. Furthermore, stasis dermatitis is more prevalent among people who are overweight.
The medical definition of “Stasis Dermatitis” is a skin irritation on the lower legs generally related to circulatory problems. Stasis refers to a stoppage or slowdown in the flow of blood (or other body fluids) and comes from the Greek word “stasis” meaning “the posture for standing.” Dermatitis is an inflammation of the skin from any number of causes.
Doctors also refer to the condition as:
- Gravitational Dermatitis
- Venous Eczema
- Venous Stasis Dermatitis
In This Article:
- What Is Stasis Dermatitis?
- What Causes Stasis Dermatitis?
- What are the Symptoms of Stasis Dermatitis?
- How is Stasis Dermatitis Diagnosed?
- How is Stasis Dermatitis Treated?
- Managing Stasis Dermatitis
- Novus Spine & Pain Center
- Stasis Dermatitis Resources
What Is Stasis Dermatitis?
Stasis dermatitis is a condition that develops in people who have poor blood circulation. It can happen because of varicose veins, congestive heart failure, or other conditions that cause fluid to buildup in the legs. Stasis dermatitis is most common in the lower limbs where reduced blood flow is most likely to develop. It can occur in just one or both legs. Stasis dermatitis can also develop in other areas of the body, but it is rare.
The lower legs are most susceptible to developing stasis dermatitis, because leg veins have built-in one-way valves to help push blood up the legs and back to the heart. As we age, these valves can weaken and may stop working properly, causing some blood to leak out of the veins and pool in the legs resulting in swelling. The pressure from the swelling prevents adequate blood and oxygen from reaching the skin.
As pressure continues to build, the pooling blood may leak into the skin causing a change, or discoloration, in the skin. If untreated, stasis dermatitis can lead to ulcers (open sores) on the skin.
The condition tends to affect people with venous insufficiency, such as varicose veins and edema (swelling). It is most often seen in the ankles but can spread up to the knees.
It is important to note that a diagnosis of venous insufficiency does not necessarily lead to the development of stasis dermatitis.
What Causes Stasis Dermatitis?
Stasis dermatitis is a direct result of poor circulation or venous insufficiency. Certain conditions, such as deep vein thrombosis, events like surgery (vein stripping, total knee arthroplasty, vein harvesting for coronary bypass), or traumatic injury, can severely damage the function of the veins in the legs and lead to venous insufficiency.
Some medical conditions that can increase the risk of developing stasis dermatitis include:
- High blood pressure.
- Varicose veins.
- Being very overweight.
- Heart conditions such as congestive heart failure.
- Kidney failure.
- A previous blood clot, especially in your leg (including deep vein thrombosis).
- Women who have had several pregnancies.
- Past surgery or injury in the area.
- Venous insufficiency (problems returning blood from the legs to the heart).
- Surgery (to the area, or removing a vein from the area).
Additionally, stasis dermatitis is more likely to develop in people who usually stand or sit for long periods of time, or who don’t get much exercise. Other traits that make it more likely to develop stasis dermatitis include age and gender.
In the United States, stasis dermatitis tends to develop mostly in people 50 years of age and older. Women are slightly more likely to develop it than men. The causes tend to point to extra weight and pregnancy, which places additional strain on the veins in the legs.
What are the Symptoms of Stasis Dermatitis?
The symptoms of stasis dermatitis may include the symptoms of venous insufficiency:
- Dull aching or heaviness in the leg.
- Pain that gets worse upon standing.
- Swelling in the leg.
Stasis dermatitis can arise quickly, causing weeping and crusting of the skin. Initially, the patient will notice swelling around the ankles. The swelling may get better after a night’s rest, but return during the day and when active.
Other symptoms of stasis dermatitis can include:
- The legs feel “heavy” when standing or walking.
- The skin around or above the ankles looks reddish, yellowish, or brown in color.
- Varicose veins – dark purple or blue twisted, bulging, veins in the legs.
- Itching and pain in the area.
- Red, swollen, painful skin or sores that ooze and crust, or look scaly.
- Thickened skin around the ankles or shins.
- The skin becomes irritated or cracks when scratched.
- Hair loss on ankles or shins.
Over time, the problems will extend upward to the calf of the leg. Some skin changes may become permanent:
- Thickening and hardening of the skin on the legs and ankles (lipodermatosclerosis).
- A bumpy or cobblestone appearance of the skin.
- Skin turns dark brown.
- Skin sores (ulcers) may develop (called a venous ulcer or stasis ulcer) most often on the inside of the ankle.
- Skin that is dry, cracked, shiny, and itchy.
- Purple or red sores on the lower legs and the tops of the feet.
- The skin becomes scaly with sores that weep and crust, and bacterial infections may develop.
- Some patients may develop eczema in other parts of the body.
If left untreated, stasis dermatitis can gradually worsen, leading to:
- Hard areas of thickened, fibrotic skin.
- Shrinking of the lower part of the leg.
- Deeply pigmented skin.
- Red and scaly skin in the affected area.
- Intense itching of the skin.
In addition, cellulitis, a serious infection affecting deeper body tissues, can develop and spread through the leg.
The effect of stasis dermatitis, along with the application of some medications, can cause the skin to become extremely sensitive and painful to touch – a condition known as contact dermatitis.
How is Stasis Dermatitis Diagnosed?
The diagnosis of stasis dermatitis is primarily from a physical examination of the affected skin. Stasis dermatitis can also be related to heart problems or other conditions that cause leg swelling. A doctor will want to check the patient’s general health, and know if there is a history of any blood clots, surgery, heart disease, or a previous injury to the affected area.
Specific medical tests may be necessary to determine why there is poor circulation. These include:
- Blood tests.
- Doppler ultrasound (to observe blood flow).
- Tests to rule out heart problems.
- Allergy testing (stasis dermatitis increases the risk of developing an allergic reaction on the skin).
How is Stasis Dermatitis Treated?
The treatment of stasis dermatitis is usually two-fold. First, to reduce the pooling of blood in the veins. The second is treating the symptoms to minimize patient discomfort.
Because circulation is the main issue, the initial conservative approach is to get the blood flowing in the legs. To improve blood flow, the doctor will advise the patient to:
- Avoid standing or sitting for long periods of time. It helps to walk around often.
- Keep the legs raised when sitting. When possible, patients should elevate their feet above the heart for 15 minutes every 2 hours and while sleeping.
- Wear compression stockings to help reduce swelling and improve blood flow.
In some cases, surgery may be necessary to repair the veins. Removal of varicose veins can be done with a minimally invasive procedure called vein stripping. If large ulcers have formed, a skin graft may be necessary.
To treat pain, redness, and swelling the doctor may prescribe medicine that can be applied topically to the ankles and legs. To reduce swelling and the amount of fluid in the legs, a diuretic may be prescribed.
A moisturizer can help with dry skin, and keep the area soft. However, choose a moisturizer without fragrance, dyes, or perfumes as these can irritate the skin even more. Petroleum jelly and thick creams are good options. Other treatment options include:
- Cool, moist compresses (only if prescribed by a doctor).
- Keep the skin clean to help prevent infection.
- Topical steroid creams or ointments to reduce inflammation.
- Zinc oxide dressings.
- Oral antibiotics to treat infections.
- Antihistamine medications (pill or cream) to help reduce itching.
Some skin care treatments can make the problem worse. Always consult a medical professional before using any over-the-counter lotions, creams, or antibiotic ointments. Things to specifically avoid include:
- Topical antibiotics, such as neomycin.
- Drying lotions, such as calamine.
- Skin products containing lanolin.
- Benzocaine and similar products that numb the skin.
The skin discoloration of stasis dermatitis often remains even after the swelling, sores, and other signs have cleared. There are treatment options that may help reduce the discoloration, which may be suggested by a dermatologist.
Managing Stasis Dermatitis
Stasis dermatitis is usually a long-term (chronic) condition. However, with a healthy lifestyle, exercise, and a balanced diet, it is possible to manage the condition. Self-care and a few changes to daily habits can help get stasis dermatitis under control, and keep it from getting worse.
Pain management doctors at the vein clinic recommend:
- Take breaks. If your job keeps you sitting or standing for long periods, take time to move. Take a brisk walk for about 10 minutes each hour.
- Elevate the legs. When possible, elevate the feet above the heart for 15 minutes every 2 hours, and while sleeping.
- Exercise. Moving increases blood flow. Before beginning any exercise routine, talk with your doctor to determine the best activities for you.
- Wear comfortable clothes. Compression stockings are a good choice for the legs; however, choose loose-fitting, cotton clothes for the rest of your body. Tight or rough fabrics like wool, polyester, and rayon can irritate the skin and affect circulation.
- Take care when bathing. Soaps and rough-textured towels can irritate stasis dermatitis.
- Use a mild, fragrance-free cleanser rather than soap. Be sure to thoroughly and gently rinse all soap off the body.
- After bathing, gently pat the water from your skin with a clean, soft towel. Allow the skin to remain slightly moist.
- While the skin is still moist, apply petroleum jelly or a thick, creamy moisturizer that is fragrance-free to the affected areas. This helps keep moisture in your skin, and can help prevent scaly skin and irritations.
Skin with stasis dermatitis is very sensitive, so avoid contact with anything that could irritate it, such as:
- Pet hair.
- Plants.
- Grass.
- Cleaning products.
- Perfume.
- Any skin care product that does not say “fragrance-free.”
- Anything else that irritates your skin.
Novus Spine & Pain Center
Novus Spine & Pain Center Vein Clinic in Lakeland, Florida specializes in treating stasis dermatitis. By using a comprehensive approach and cutting-edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Stasis Dermatitis Resources
What is Stasis Dermatis (Web MD)
What is Venous Stasis Dermatitis? (Web MD)
How is Stasis Dermatitis Treated? (Web MD)
How does stasis dermatitis develop? (Web MD)
Stasis Dermatitis (Medscape)
Stasis Dermatitis and Ulcers (Medline Plus)
Stasis Dermatitis (Mayo Clinic)
Other Dermatitis Conditions (Johns Hopkins)
Medical Definition of Stasis dermatitis (MedicineNet)
Stasis Dermatitis (American Academy of Dermatology Association)
Varicose eczema, or stasis dermatitis: What you need to know (Medical News Today)
Vein Ligation and Stripping (WebMD)
Updated: February 21, 2021

