 There are more than 200,000 cases of spinal stenosis in the U.S. each year, usually affecting the neck or lower back. Patients suffering from spinal stenosis can experience numbness and back pain, and may suffer from sciatica, foot drop, difficulty standing or walking, and loss of bladder or bowel control, depending on the location of the stenosis.
There are more than 200,000 cases of spinal stenosis in the U.S. each year, usually affecting the neck or lower back. Patients suffering from spinal stenosis can experience numbness and back pain, and may suffer from sciatica, foot drop, difficulty standing or walking, and loss of bladder or bowel control, depending on the location of the stenosis.
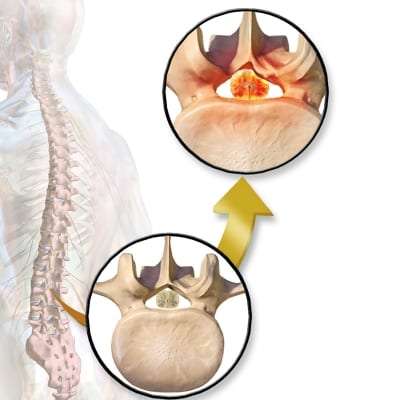
What Is Spinal Stenosis?
Spinal stenosis is a narrowing of the spinal canal. When the spinal canal narrows, it presses on the spinal cord and nerves leading to the arms and legs.
Often affecting people over age 50, spinal stenosis is frequently the result of wear-and-tear changes in the spine caused by osteoarthritis. Spinal stenosis can also be congenital or the result of trauma. There is no cure for stenosis (narrowing) of the spinal canal; however, the pain management specialists at Novus Spine and Pain Center in Lakeland, Florida can help patients live normal lives.
The most common types of spinal stenosis are lumbar (lower) back and cervical (neck) stenosis. Lumbar spinal stenosis is most common, but cervical spinal stenosis is more dangerous because compression of the spinal cord can lead to weakness and even paralysis.
Patients suffering from spinal stenosis typically experience persistent pain in the lower back and lower extremities. Some people may have no signs or symptoms related to the stenosis, while others may experience pain, tingling, numbness, and muscle weakness in the legs, arms, or torso. Some patients may experience difficulty walking, decreased sensation in the lower extremities, and decreased physical activity. In some cases, spinal stenosis may cause problems with bladder or bowel function.
What Causes Spinal Stenosis?
Spinal stenosis is most commonly caused by everyday ‘wear-and-tear’ of the body as it ages, resulting from osteoarthritis (breakdown of joint cartilage) in the spine. Osteoarthritis can lead to changes in the discs of the spine, a thickening of the ligaments, and bone spurs that may place pressure on the spinal cord and nerves.
For people born with spinal stenosis or diseases that lead to it, the condition usually starts to cause problems between the ages of 30 and 50. Other causes of spinal stenosis include:
- Overgrowth of bone. Paget’s disease, a bone disease that usually affects adults that cause the overgrowth of bone in the spine.
- Herniated discs.The soft cushions that act as shock absorbers between the vertebrae in the spine tend to dry with age. Cracks in a disc’s exterior may allow some of the soft inner material to escape and press on the spinal cord or nerves.
- Thickened ligaments.The tough cords that help hold the bones of the spine together can become stiff and thickened as one ages. These thickened ligaments may protrude into the spinal canal and press on the spinal cord and nerves.
- Abnormal growths that form inside the spinal canal within the membranes that cover the spinal cord or in the space between the spinal cord and vertebrae.
- Spinal injuries. Car accidents and other types of major trauma can dislocate or fracture some of the vertebrae. Displaced bone from a spinal fracture may damage the contents of the spinal canal. Swelling of adjacent tissue immediately following back surgery can also put pressure on the spinal cord or nerves.
What are the Symptoms of Spinal Stenosis?
Symptoms of spinal stenosis vary, depending on the location and severity of the stenosis. When the symptoms first appear, they often begin gradually and then worsen with time. The condition usually affects the neck or lower back. However, not everyone has symptoms; in some patients, X-rays may show evidence of spinal stenosis, but the patient does not experience any pain.
In some patients, the symptoms begin as sciatica. These patients may find that the pain worsens when standing upright due to compression of vertebrae which may result in difficultly standing or walking. In extreme cases, the patient may suffer from a loss of bladder or bowel control because of weakened nerves leading to the bladder or bowel.
Symptoms caused by compression of the spinal cord (myelopathy) can include:
- Worsening balance.
- Falling.
- Dropping objects.
- Difficulty buttoning buttons or picking up small coins.
- Loss of bowel or bladder control.
Symptoms caused by compression of the nerves (radiculopathy) can include:
- Pain.
- Numbness.
- Tingling.
- Weakness along the path of the compressed nerve.
When stenosis develops in the neck (cervical stenosis), there can be compression of the spinal cord and the nerves that travel into the arms and hands. This can cause symptoms of:
- Numbness.
- Tingling.
- Weakness or cramping in the arms and hands.
When the stenosis develops in the lower back (lumbar stenosis), there is compression of the nerves that travel into the legs and feet. This can cause:
- Pain.
- Numbness.
- Tingling.
- Weakness or cramping in the legs and feet.
How is Spinal Stenosis Diagnosed?
Diagnosis begins with a complete medical history which includes questions about the patient’s symptoms. Additionally, the doctor will want to know which actions or movements increase or lessen the pain.
A review of a patient’s medical history is followed by a physical examination to test muscle strength, reflexes, sensation, balance, and circulation. Identifying the patient’s symptoms helps determine which nerves are affected by the stenosis.
Depending on the patient, imaging tests may be needed to help pinpoint the spinal stenosis. These tests may include:
- X-rays. The X-ray can reveal bony changes, such as bone spurs that may be narrowing the space within the spinal canal.
- Magnetic resonance imaging (MRI). In most cases, this is the primary test for diagnosing spinal stenosis. The test can detect damage to discs and ligaments, as well as the presence of tumors. Most importantly, an MRI can reveal pressure points on the spinal cord or nerves.
- CT myelogram. Computerized tomography (CT) combines X-ray images taken from many different angles to produce detailed, cross-sectional images of the body. In a CT myelogram, an injection of a contrast dye helps outline the spinal cord and nerves to reveal possible herniated discs, bone spurs or tumors.
A doctor may also order a nerve conduction study or an EMG (electromyography) to look for nerve damage caused by spinal stenosis.
How is Spinal Stenosis Treated?
In some cases, it is possible to treat stenosis with a non-surgical approach. A combination of exercise, lifestyle changes, heat and cold therapy, injections, and oral medication can help control the symptoms of spinal stenosis.
Some of the options available for treating spinal stenosis are:
- Medications
- NSAIDs (ibuprofen-like drugs), membrane stabilizing drugs, and other analgesics are often used in the management of pain associated with spinal stenosis.
- Muscle relaxants. Medications that can calm muscle spasms that are occasionally associated with spinal stenosis.
- Antidepressants. Nightly doses of some antidepressant medications have been shown to help ease chronic pain.
- Anti-seizure drugs. Some anti-seizure drugs are used to reduce pain caused by damaged nerves.
- Opioids. Medications that contain codeine-related drugs can only be used for a short time because they are habit-forming.
- Epidural steroid injections. This procedure involves injecting a medication into the epidural space, where irritated nerve roots are located. This injection includes both a long-lasting steroid and a local anesthetic.
- Percutaneous adhesiolysis. The procedure, also known as the Racz procedure, is proven effective in removing excessive scar tissue in the epidural space. Scar tissue originates from inflammation, irritation, and often surgery.
- Spinal cord stimulation (SCS). Spinal cord stimulation in often effective in treating spinal stenosis. SCS involves implanting an electrical device that decreases the perception of pain by confusing the spinal cord and brain pain processing centers. Tingling electrical signals replace the pain signals.
- Alternative treatments. Some patients find relief with nontraditional therapies, such as chiropractic, acupuncture, massage, and yoga. Acupuncture has been shown to be more effective in treating neck and back pain than inactive treatments. Alternative treatments can be beneficial for patients who are unable to undergo surgical treatment due to existing health conditions.
- Injections of a “nerve block” can stop the pain for a time.
- Regular activity improves flexibility, strength, and balance. Sometimes we recommend a physical therapist to help the patient.
- Assistive devices. To help the patient move, sometimes a brace, a corset, or a walker is beneficial in easing the pain associated with movement.
- Surgical treatments. When all conservative measures have been exhausted, and the symptoms continue to be severe, a more invasive surgical procedure may be necessary to take pressure off the spinal cord and surrounding nerves. Minimally invasive spine surgery may resolve stenosis with a lower risk for complications and a potentially faster recovery time than conventional open surgery procedures.
Can you Avoid Spinal Stenosis?
Many of the causes of spinal stenosis cannot be prevented, because they are due to age-related issues such as degenerative arthritis. But on the positive side, individuals can help limit the symptoms by staying fit and in good overall health.
While many people will not develop spinal stenosis, certain people are more likely to develop this condition than others. Besides family history and genetics, you may be at an increased risk of developing spinal stenosis if you place a greater demand on your back.
There are many potential reasons you may begin to experience increasing pain in your neck or back, or experience numbness and tingling in your arms and legs. If the symptoms last longer than six weeks, if there is increasing weakness in your arms, or if problems controlling your bowel or bladder persist, seek immediate medical attention.
Novus Spine & Pain Center
Novus Spine and Pain Center is in Lakeland, Florida, and specializes in treating spinal stenosis. By using a comprehensive approach and cutting edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Spinal Stenosis Resources
Spinal Stenosis (Mayo Clinic)
Spinal Stenosis (Johns Hopkins)
What is Spinal Stenosis? (WebMD)
Spinal Stenosis (eMedicine Health)
Spinal Stenosis (Wikipedia)
Image Credit: Wikipedia/Blausen.com staff. “Blausen gallery 2014“.
Updated: November 15, 2021

