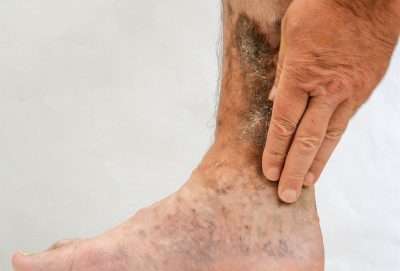
 Venous ulcers are open skin sores that can affect any area of the body but most often occur on the legs. About 1% of Americans have venous ulcers. They’re more common in older people, particularly women, and more likely to occur with people who have varicose veins. Others with an increased chance of developing a venous ulcer include:
Venous ulcers are open skin sores that can affect any area of the body but most often occur on the legs. About 1% of Americans have venous ulcers. They’re more common in older people, particularly women, and more likely to occur with people who have varicose veins. Others with an increased chance of developing a venous ulcer include:
- People who have suffered previous leg injuries.
- People who smoke.
- The overweight or obese.
- Anyone with a circulation problem such as blood clots or phlebitis (inflammation of a vein that can result in painful swelling).
Venous ulcers are sometimes called venous insufficiency ulcers, stasis leg ulcers, or venous leg ulcers.
What Are Venous Ulcers?
A venous ulcer is a sore, usually occurring on the leg, that is slow to heal because of blood flow (circulation) problems in the veins. Most venous ulcers occur on the lower leg, above the ankle.
When leg veins do not push blood back up to the heart as they should, the blood backs up (pools), creating extra pressure in the veins. Because of the continuous pressure, venous ulcers can linger anywhere from a few weeks to years. If left untreated, the affected area can cause an open sore to form, which can lead to more serious problems.
What Causes Venous Ulcers?
Any condition that causes blood to pool in the veins of the leg is a potential cause of venous ulcers. The pooling blood in the leg can prevent nutrients and oxygen from getting to surrounding tissues. This condition can cause cells to die, damage the tissue, and form an ulcer (wound). In some cases, the ulcer may be painful.
Some of the conditions that can cause venous ulcers are venous insufficiency, varicose veins, deep vein thrombosis, and heart failure. Other medical conditions that can cause venous ulcers include:
- Poor circulation and blood clotting disorders that may be related to atherosclerosis.
- Diabetes.
- Renal (kidney) failure.
- Hypertension (treated or untreated).
- Lymphedema (swelling resulting from impaired flow of the lymphatic system).
- Inflammatory diseases including vasculitis, lupus, scleroderma, and other rheumatological conditions.
- A history of smoking (either current or past).
- Pressure caused by lying in one position too long.
- Genetics (ulcers may be hereditary).
- A malignancy (tumor or cancerous mass).
- Infections.
Other medical conditions such as high cholesterol, heart disease, high blood pressure, sickle cell anemia, and bowel disorders can also cause venous ulcers. Certain medications can also cause venous ulcers in some people.
What Are the Symptoms of Venous Ulcers?
Venous ulcers are sores in the skin, usually on the inside of the leg just above the ankle. The ulcers are also commonly associated with stasis dermatitis and venous insufficiency.
A patient suffering from a venous ulcer will usually experience a swollen leg, often with a burning feeling around the sore. A typical complication associated with venous ulcers is an infection of the affected tissue. Other signs and symptoms of venous ulcers include:
- The leg has a feeling of heaviness and cramping.
- There is general leg pain.
- The sore is shallow with a red base, sometimes covered by yellow tissue.
- A sore with unevenly shaped borders.
- The skin surrounding the sore may be shiny, tight, feel warm, or even hot.
- If the sore becomes infected, it may have a foul odor, and pus may drain from the wound.
Typically, the ulcer itself is relatively painless. If there is pain, it is from an infection or swelling (edema). In some cases, the entire leg can become swollen, making the skin hardened (a sign of blood pooling) and have a reddish-brown appearance.
How Are Venous Ulcers Treated?
Venous ulcers need proper care and treatment to heal and prevent infection. The Lakeland pain management doctors at the Novus Spine & Pain Center Vein Clinic work with each patient to determine the cause of the ulcer and develop an individualized treatment plan. Primary treatment goals, in addition to healing, are to relieve pain and speed recovery. Treatment often includes focusing on the circulatory or vein problems causing the ulcers.
The most common treatment to reduce the swelling is a compression bandage or stocking, which can help improve blood circulation in the legs. The improvement in circulation helps boost the body’s ability to heal the sore. The type of bandage will vary with each patient. Some compression bandages may require the patient to wear them continuously, with a doctor replacing them every few days. Others are worn only during the day, with the patient putting them on and removing them.
In treating venous ulcers, it is essential to keep the site infection-free. Prescribed medication may be applied under the bandages or stockings to help during the healing process. Should the venous ulcer become infected by bacteria, the doctor may prescribe antibiotics to kill the infection.
Other home care treatment options include:
- Apply a dressing to the ulcer and change as directed by the doctor.
- Apply an antibacterial ointment or another topical medicine to prevent or treat an infection.
- Avoiding products (soaps and detergents) and clothing that can cause skin sensitivity.
- Clean the wound regularly.
- Place feet above the heart as often as possible to help circulation. Typically, a half-hour at a time, 3 or 4 times a day. For example, lie down with feet elevated on pillows.
- Take a walk or exercise every day. Regular activity helps improve blood flow.
- Take oral antibiotic medicines to prevent or treat an infection.
- Wear appropriate shoes.
- Drink plenty of fluids.
- Follow a healthy diet that includes plenty of fruits and vegetables.
Most venous ulcers heal after 3 or 4 months of treatment. However, some can take longer or require a skin graft to close the opening in the skin. However, some ulcers may never completely clear up.
Novus Spine & Pain Center
Dr. Torres established Novus Spine & Pain Center in Lakeland, Florida, with the goal of providing the highest quality pain management care to every patient. Whether pain is the result of an injury or from another condition, Dr. Torres offers many different treatment options.
Novus Spine & Pain Center utilizes a comprehensive approach and cutting-edge therapies to restore normal function and allow patients to regain an active lifestyle while minimizing the need for opiates. As our patient, you are our top priority. Our goal is to help you achieve the best possible quality of life.
Our Mission Statement: To provide the best quality of life to people suffering from pain by providing state-of-the-art treatments, knowledge and skill, compassion, and respect for all.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-473-7849.
Venous Ulcers Resources
More information about Venous Ulcers is available from:
American Venous Forum
2800 West Higgins Road, Suite 440
Hoffman Estates, IL 60169
Tel: 727.350.1580
Email: [email protected]
Society for Vascular Surgery
633 N. Saint Clair St., 22nd Floor
Chicago, IL 60611
Telephone: 312-334-2300 / 800-258-7188
Email: [email protected]
What Is a Venous Skin Ulcer (WebMD)
Venous Ulcers (Johns Hopkins)
Subfascial Endoscopic Perforator Surgery (Stanford Health Care)
Venous Ulcers – Self-Care (MedlinePlus)
Venous Leg Ulcers (American Family Physician)
Venous Insufficiency Ulcers (Wound Source)
Leg and Foot Ulcers (Cleveland Clinic)
Ankle-brachial index (Mayo Clinic)
Doppler ultrasound: What is it used for? (Mayo Clinic)
Lymphedema (MedicineNet)

