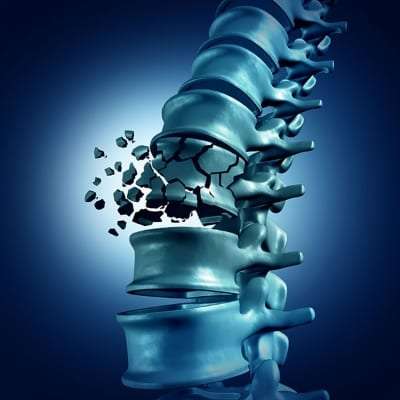
 Vertebral body fractures and vertebral compression fractures are often a source of debilitating pain that prevents many older adults from enjoying a healthy and active lifestyle. Fortunately, there are several treatments available to relieve the pain, and minimally invasive procedures to repair spinal fractures.
Vertebral body fractures and vertebral compression fractures are often a source of debilitating pain that prevents many older adults from enjoying a healthy and active lifestyle. Fortunately, there are several treatments available to relieve the pain, and minimally invasive procedures to repair spinal fractures.
What Are Vertebral Body Fractures & Vertebral Compression Fractures?
The vertebral body is the thick oval segment of bone that forms the front of the vertebrae (bones of the spine) and protects the spinal cord. The vertebral body is the large, round weight bearing portion of the vertebrae, and consists of an outer shell of solid bone and an inner network of porous spongy bone.
A vertebral body fracture is a splintering of the vertebrae that results in a collapse of the vertebral body.
A vertebral compression fracture occurs when one or more bones in the spine weaken and compress, typically from the loss of bone mass (osteoporosis); but can also occur after a fall, cough, or lifting a heavy object.
What Causes Vertebral Body Fractures & Vertebral Compression Fractures?
Healthy bones are designed to provide strength, flexibility, and support to the spinal canal. They can withstand reasonable amounts of pressure. However, if the force placed on a vertebra exceeds the threshold of normal pressure, it may fracture and collapse. Typically, vertebral body fractures are the result of severe trauma that exerts an excessive vertical force on the spine (such as an accident, or a fall). This type of accident typically crushes the vertebrae in the thoracic (middle portion) of the spine.
Vertebral fractures are the most common fracture in elderly patients, usually resulting from compression or trauma. As we age, our bones become thinner and weaker, and are more prone to fracture.
Both women and men with osteoporosis have much higher chances of suffering from a spinal fracture, but women age 50 and older are most likely to suffer from spinal fractures. Furthermore, it is estimated that by age 80, about 40% of women will have a spinal fracture. Certain types of cancers that spread to the vertebrae can also result in compression fractures.
What are the Symptoms of Vertebral Body Fractures & Vertebral Compression Fractures?
The pain from an injury to the spinal cord and nerves from a vertebral body fracture varies. Bone fragments from the fracture can bruise the spinal cord causing partial nerve injury and even paralysis.
The main symptom of a vertebral fracture is back pain. The pain may start gradually and get worse over time. In some cases, the onset of pain may begin suddenly. Although many patients report some degree of back pain following a vertebral fracture, others may not have any immediate symptoms.
Fractures in the lower spine often cause greater pain and difficulty in moving, than fractures in the upper spine. It is also possible to fracture more than one vertebrae in the spine. When a vertebra is fractured, the body has more difficulty supporting the weight of the spine, which affects how the body functions.
Over time, symptoms of a spinal fracture can include:
- Pain: Pain tends to be in the lower back, but may occur in the middle or upper back, and even the neck. The pain often worsens when standing or walking, so patients may get relief when reclining. Some patients may also experience hip, abdominal, or thigh pain.
- There may be pain or difficulty when bending or twisting the body.
- Numbness, tingling, and weakness: Such symptoms could indicate the nerves at the fracture site are pinched or damaged.
- Incontinence or inability to urinate (urinary retention): If these symptoms are present, the fracture may be pressing on the spinal cord.
- A curved or stooped shape of the spine.
- Height loss: Each fracture of a vertebrae results in the shortening of the spine. Eventually, with the collapse of several vertebrae, the patient will look noticeably shorter.
- Kyphosis (curved back): With each vertebral compression fracture, the spine tends to curve more, bending forward. Eventually, this causes neck and back pain, as the body tries to adapt to changes in the spine.
- Stomach problems: A shorter spine can compress the stomach, which can cause digestive problems like constipation, loss of appetite, and weight loss.
- Hip pain: A shorter spine can also move the rib cage closer to the hipbones, resulting in severe pain if the bones rub against each other.
- Breathing problems: In cases of a severely compressed spine, there is less room for the lungs to fully inflate with air, which leads to breathing troubles.
Symptoms are different for everyone, so it is important to consult a physician for pain that quickly worsens or does not subside after a few days.
In many cases, back pain from vertebral fractures is relieved by lying down and worsens with activity. Along with back pain, spinal compression fractures can also cause additional pain when performing simple activities that might cause the slightest back strain. Some of these activities include:
- Lifting a bag of groceries.
- Bending over to pick something off the floor.
- Slipping on a rug or making a misstep.
- Lifting anything from the trunk of a car.
- Lifting a mattress corner when changing bed linens.
How are Vertebral Body Fractures & Vertebral Compression Fractures Diagnosed?
A medical history and physical exam are the first steps in diagnosing a vertebral fracture. The physical exam will uncover tenderness at the fractured vertebrae, as well as a possible unusual curving of the spine (kyphosis). However, depending on the outcome of the exam, your physician may order additional imaging test such as an MRI, CT scan, or a bone scan.
- X-rays: X-rays are helpful in screening for fractures, but hairline fractures and nondisplaced fractures can be difficult to detect. In many cases, an X-ray alone may not show a fracture or the classic wedge-shaped vertebral body.
- Computed tomography (CT) scan of the spine: CT scans readily detect bone fractures and help determine the extent of any fracture.
- Magnetic resonance imaging (MRI): An MRI is the most sensitive test for detecting lesions of neural tissue and bone. The MRI is usually the study of choice for determining the extent of damage to the spinal cord. An MRI is helpful in revealing pressure points on the spinal cord and nerves.
How are Vertebral Body Fractures & Vertebral Compression Fractures Treated?
Treatment for vertebral compression fractures is as varied as the range of pain associated with the fractures. A conservative approach may include medications, physical therapy, and lifestyle changes. However, more advanced procedures may be necessary in some cases. If the fracture is the result of osteoporosis, treatment to stop the softening of the bones and protect the rest of the skeletal frame may be necessary.
Treatment may include a short period of bed rest; however, prolonged inactivity can worsen the condition. For this reason, the patient is encouraged to move around as soon as possible. Sometimes a physical therapist is necessary to supervise exercises to help the injury heal. Stretching and other exercises are important to help decrease further osteoporosis, while also strengthening muscles that support the back.
In some cases, the spine may require support, and a brace is used to aid healing by preventing rotational movement and bending of the spine.
The patient will probably receive medication to relieve pain while the fracture heals. The use of NSAIDs and analgesics are available for the management of pain. Although these may help ease the discomfort, they do not correct the underlying problem causing the pain.
In some cases, a minimally invasive procedure is necessary to repair the fracture, and for spinal stabilization. The two most common procedures are vertebroplasty and kyphoplasty, which can significantly reduce pain and improve mobility for patients suffering from vertebral fractures.
Vertebroplasty is a procedure involving injecting an acrylic cement or biomaterial compound into the vertebrae with the fracture. The material hardens, like cement, stabilizing and strengthening the compressed vertebrae. The cement provides support and allows for healing.
Vertebroplasty is an outpatient procedure, usually performed while the patient is awake but sedated. A local anesthetic numbs the back where a small incision is made. Fluoroscopy (which converts x-rays into video images) is used to guide the procedure, and the doctor injects bone cement into the damaged vertebrae with a needle. The procedure usually takes about 40 minutes for each vertebra.
Kyphoplasty is similar to vertebroplasty, except it utilizes the injection of an inflatable balloon into the damaged vertebrae. Once in place, the balloon is slowly inflated to elevate the fracture, returning the pieces to a more normal position, while also compacting the soft inner bone to create a cavity inside the vertebrae.
Ways to Avoid Vertebral Body Fractures & Vertebral Compression Fractures
Research indicates diagnosing and treating osteoporosis helps reduces the incidence of spinal compression fractures. Consistent exercise and activity that assist in strengthening muscles and improving flexibility can also improve the back pain associated with osteoporosis.
Some ways to prevent osteoporosis include:
- Diet: Eat a well-balanced diet that is calcium-rich.
- Activity: Regular exercise that includes weight-bearing and strength-training exercise can help increase bone strength.
- Stop smoking: Studies show that smoking tobacco weakens bones.
- Supplements: Anyone at risk for osteoporosis should consider taking calcium and vitamin D supplements.
- Estrogen replacement: Estrogen replacement therapy in women past the age of menopause may help prevent osteoporosis. Medications seem to reduce the development of osteoporosis when taken along with appropriate doses of calcium and vitamin D. Supplements may also decreasing the rate of bone loss in women who already have osteoporosis.
Reduce steroids: Older patients on a daily steroid therapy should speak to their doctor about the possibility of reducing the dosage. Decreasing the steroid dose reduces the chance of developing osteoporosis. There may be other medications reducing the amount of steroids needed.
Novus Spine & Pain Center
Novus Spine & Pain Center specializes pain management, and treatment of vertebral body fractures and vertebral compression fractures. By using a comprehensive approach and cutting edge therapies, we work together with patients to restore function and regain an active lifestyle, while minimizing the need for opiates.
To schedule an appointment, please contact us online, request a call back, or call our office at 863-583-4445.
Resources
Vertebral Fracture (eMedicine.com)
Vertebral Compression Fracture (eMedicineHealth.com)
Burst Fractures: Defined and Diagnosed (Spine Universe)
When Back Pain Is a Spine Compression Fracture (Spine Health.com)
Osteoporosis and Spine Fractures (WebMD)
Vertebroplasty (Mayo Clinic)
Vertebral Compression Fracture (Wikipedia)
Updated: February 22, 2020

