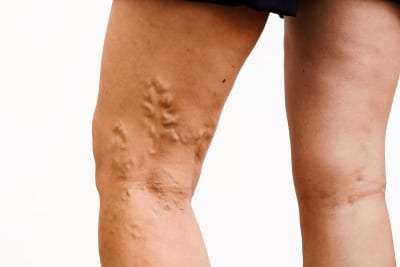
 Varicose veins affect around 25% of adults in the United States. Most varicose veins are not a health issue, but they should not be ignored. Varicose veins can cause fatigue of the legs, swelling, and general discomfort. They can lead to a blood clot or other circulatory problems and warn of long-term health risks.
Varicose veins affect around 25% of adults in the United States. Most varicose veins are not a health issue, but they should not be ignored. Varicose veins can cause fatigue of the legs, swelling, and general discomfort. They can lead to a blood clot or other circulatory problems and warn of long-term health risks.
The veins most likely to become varicose are in the legs and feet because veins in the lower body are under increased pressure to help pump blood back to the heart. However, any vein may become varicose.
What Are Varicose Veins?
Varicose veins are enlarged, swollen, and twisting veins that bulge from blood pooling in them. When valves in the veins fail to work correctly, blood can pool or flows in the wrong direction, causing a vein to bulge. When veins bulge, they become visible through the skin, often appearing blue or dark purple.
Varicose veins can cause considerable discomfort. In severe cases, a varicose vein may rupture or develop into varicose ulcers (open sores) on the skin and require treatment.
Small “spider veins,” a milder form of varicose veins, also can appear on the skin’s surface. These often look like short, fine lines, in “starburst” clusters, or a web-like maze. Spider veins are most common in the thighs, calves, ankles, and feet. They may also appear on the face.
What Causes Varicose Veins?
Varicose veins are caused by increased blood pressure in the veins near the skin’s surface. Arteries carry blood from the heart to the rest of the body. Veins return blood to the heart, allowing blood to recirculate. To return blood to the heart, the veins in the legs need to work against gravity. Within the veins are tiny valves that open as blood flows toward the heart, then close to stop the backflow of blood. Muscle contractions in the lower legs and elastic vein walls also help the blood return to the heart.
In some instances of varicose veins, a weakness of vein valves can cause poor circulation. In other cases, a weakness in the vein wall may cause pooling of the blood. As the blood pools, the vein becomes engorged and forms spider veins, which lead to varicose veins. Varicose veins can also result from a disease such as phlebitis (inflammation of the veins) or congenital vein abnormalities.
Some of the factors that can increase blood pressure within veins and result in varicose veins include:
- Age. As we grow older, the veins tend to lose elasticity and begin to stretch. The stretching causes the valves in the veins to become weak and allow blood to pool.
- Sex. 70 to 80% of the patients treated for varicose veins are women.
- Lack of activity. Standing or sitting for a long time, especially with legs bent or crossed, may raise the risk for varicose veins. Staying in one position for a long time can force the veins to work harder to pump blood to the heart. Fortunately, merely crossing the legs or wearing high heels does NOT cause varicose veins.
- Family history. Varicose veins may be an inherited trait. About half of all people who have varicose veins have a family history of them.
- Hormone changes. Changes in hormone levels brought on by puberty, contraceptives, pregnancy, menopause, and hormone replacement therapy are all risk factors for varicose veins.
- Leg injury. Traumatic damage to the valves in your veins or blood clots can weaken a vein’s ability to move blood back to the heart, increasing the risk for varicose veins.
- Obesity. Being overweight places added pressure on the veins. Anything that increases pressure in the abdomen can lead to varicose veins.
- Pregnancy. Pregnancy increases the volume of blood in the body but can decrease the flow of blood from the legs. This circulatory change is designed to support the growing fetus but can produce enlarged veins in the legs. Changes in hormones during pregnancy also may play a role. Varicose veins that develop during pregnancy generally improve without medical treatment after delivery.
- Smoking. The nicotine in cigarette smoke raises blood pressure and heart rate, which can lead to varicose veins.
How Are Varicose Veins Treated?
The treatment of varicose veins is often sought for cosmetic reasons. In many cases, medical treatment is not necessary if there are no symptoms. However, varicose veins may become worse without treatment. Severe cases of varicose veins, especially those involving ulcers, typically require treatment.
Frequently, the treatment for varicose veins is the elimination of “bad” veins. This forces blood to flow through the remaining healthy veins. Various methods can be employed to eliminate the problem veins. Thanks to less invasive procedures, varicose veins can generally be treated on an outpatient basis. Some of the procedures available include:
- Ambulatory phlebectomy. Smaller varicose veins are removed through a series of tiny skin punctures. Only the parts of the leg treated require numbing.
- Catheter-assisted procedures using radiofrequency or laser energy. A thin tube (catheter) is inserted into a varicose vein. The tip of the catheter is heated using either radiofrequency or laser energy. As the catheter is pulled out, the heat destroys the vein by causing it to collapse and seal shut.
- Sclerotherapy. A common procedure that is effective in eliminating most spider veins and some varicose veins is sclerotherapy. A liquid solution is injected directly into the affected vein, which causes the vein to collapse and eventually fade away. The procedure requires no anesthesia.
- Laser therapy. A laser closes off smaller varicose veins, resulting in the vein slowly fading and disappearing.
- High ligation and vein stripping. This procedure involves tying off a vein and removing the vein through a small incision. Removing the vein will not adversely affect circulation in the leg because veins deeper in the leg take care of the larger blood volume.
Following treatment for small varicose veins, patients can usually expect to see results in three to six weeks. Larger veins may require three to four months. In some cases, multiple treatments may be necessary to achieve the desired results. Generally, veins that respond to treatment do not come back, but new varicose veins may develop.
Is It Possible to Prevent Varicose Veins?
Venous disease is generally progressive, and there is no way to completely prevent varicose veins. However, improving circulation and muscle tone can reduce the risk of developing varicose veins.
Self-care measures that can help prevent or slow the development of varicose veins, while helping decrease the discomfort of varicose veins, include:
- Avoid crossing legs. Some doctors believe this position can increase circulation problems.
- Avoid long periods of sitting or standing. Make a point of changing the body’s position frequently to encourage blood flow. If it is necessary to sit or stand for an extended period, occasional flexing (bending) of the legs can help keep blood circulating.
- Elevate the legs. To improve blood circulation in the legs, elevate the feet above the level of the heart 3 or 4 times a day for about 15 minutes at a time. Lie down with lower legs resting on three or four pillows. For mild to moderate varicose veins, elevating the legs can help reduce leg swelling and may also relieve other symptoms.
- Exercise. Get moving! Walking is a great way to encourage blood circulation in the legs.
- Weight and diet. Shedding excess pounds takes unnecessary pressure off the veins. A high-fiber, low-salt diet can help prevent swelling caused by water retention.
- Shoes and clothing. Avoid high heels. Shoes with low heels work calf muscles more and are better for the veins. Avoid wearing tight clothes around the waist, legs, and groin that can reduce blood flow to the legs.
- Compression (support) stockings. Elastic stockings that squeeze the leg veins and prevent blood from pooling can help alleviate mild symptoms. Compression stockings are most effective when worn daily.
Novus Spine & Pain Center
Dr. Torres established Novus Spine & Pain Center in Lakeland, Florida, with a goal of providing the highest quality pain management care to every patient. Whether pain is the result of an injury or from another condition, Dr. Torres offers many different treatment options.
Novus Spine & Pain Center utilizes a comprehensive approach and cutting-edge therapies to restore normal function and allow patients to regain an active lifestyle while minimizing the need for opiates. As our patient, you are our top priority. Our goal is to help you achieve the best possible quality of life.
Our Mission Statement: To provide the best quality of life to people suffering from pain, by providing state of the art treatments, knowledge and skill, compassion, and respect for all.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-583-4445.
Varicose Veins Resources
What are Spider Veins (WebMD)
Varicose Veins and Spider Veins (WebMD)
Spider Veins and Varicose Veins (WebMD)
Varicose Veins (Mayo Clinic)
Spider veins: How are they removed? (Mayo Clinic)
Sclerotherapy (Mayo Clinic)
Pregnancy and Skin Changes (Johns Hopkins)
Varicose Veins (Johns Hopkins)
Spider and Varicose Veins (OnHealth)
9 Things You Need To Know About Varicose And Spider Veins (Woman’s Day)
Varicose Veins (Cedars-Sinai)
What Can I Do About Varicose Veins? (Medical News Today)
Varicose Veins (NIH/National Heart, Lung, and Blood Institute)
Updated: 9/23/22

