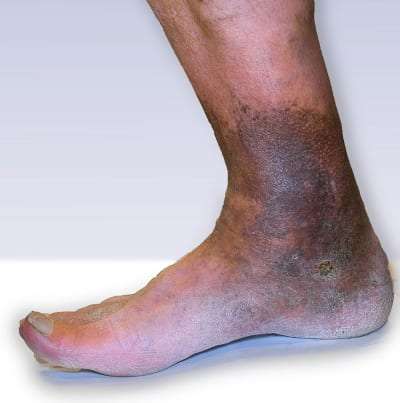
 Venous insufficiency is a condition that occurs when veins in the legs do not work effectively in returning blood to the heart. With this condition, the blood “pools” or collects in the veins. An early symptom of venous insufficiency is swelling (edema) in the ankles and feet. The condition is quite common and often becomes a chronic condition.
Venous insufficiency is a condition that occurs when veins in the legs do not work effectively in returning blood to the heart. With this condition, the blood “pools” or collects in the veins. An early symptom of venous insufficiency is swelling (edema) in the ankles and feet. The condition is quite common and often becomes a chronic condition.
In general, venous insufficiency does not pose a serious health threat; however, it can become disabling and cause pain as the condition worsens. In addition, if allowed to continue untreated, chronic venous insufficiency (CVI) can lead to skin changes, skin ulcers, and infections.
According to the Society for Vascular Surgery, CVI affects up to 40% of the U.S. population. Hippocrates recognized the condition in ancient times and wrote of using bandaging as a treatment.
What Is Venous Insufficiency?
Arteries carry blood from the heart to the rest of the body. Veins carry blood back to the heart. In the legs, veins have one-way valves to keep blood from flowing backward. When the vein walls and valves fail to work correctly, pumping blood back to the heart is not as effective as with healthy veins. The condition is called venous insufficiency.
When a person has venous insufficiency, the blood will pool (stasis) in the veins of the legs instead of flowing back to the heart effectively. If chronic venous insufficiency is not treated, it can result in pain and swelling. In addition, leg ulcers may develop.
Venous insufficiency is more common in women than in men. It is also more likely to occur in women between the ages of 40 and 49. However, men between the ages of 70 and 79 are also likely to develop the condition.
What Causes Venous Insufficiency?
Several factors can lead to venous insufficiency, though it’s most commonly caused by blood clots (deep vein thrombosis) and varicose veins. In addition, when there is an obstruction to blood flow, such as is the case with a blood clot, blood builds up below the clot and leads to venous insufficiency.
In varicose veins, the valves are impaired or can be missing causing blood to leak through a damaged valve. In some cases, weak leg muscles that normally help squeeze blood forward can also contribute to venous insufficiency. Lack of exercise can be a contributing factor to venous insufficiency. Additionally, sitting or standing for long periods can raise the pressure in the veins and may weaken the valves. For unknown reasons, the valves in veins can become ineffective after an extended period of standing.
Individuals who have suffered leg trauma due to an injury, surgery, or previous blood clots are more likely to develop the condition. Other causes of chronic venous insufficiency include, but are not limited to:
- A history of blood clots.
- Over the age of 50.
- Cancer.
- Deep vein thrombosis (DVT), a blood clot in a deep vein, often in the calf or thigh.
- Family history of venous insufficiency.
- Extended times of high blood pressure in leg veins due to sitting or standing for prolonged periods.
- Obesity.
- Pregnant or have been pregnant more than once.
- Smoking.
- Swelling of a superficial vein (phlebitis).
- Varicose veins or a family history of varicose veins.
Chronic venous insufficiency that develops because of deep vein thrombosis (DVT) is also known as post-thrombotic syndrome. As many as 30 percent of people with a DVT will develop this problem within ten years after diagnosis.
What are the Symptoms of Venous Insufficiency?
Some venous insufficiency symptoms can resemble other conditions, often making self-diagnosis problematic. Most symptoms do tend to be mild and not a threat to the health of the legs. However, it is best to see a vein specialist for proper diagnosis and treatment if symptoms are present.
Without treatment, the pressure and swelling in the blood vessels may burst the tiny blood vessels (capillaries) in the legs. If the capillaries burst, the skin may turn reddish-brown, especially near the ankles. In addition, the condition can lead to swelling and ulcers. If ulcers develop, they are difficult to heal and can become infected, causing additional problems. Ulcers are less likely to develop if treatment begins early.
Other symptoms of chronic venous insufficiency can include:
- Aching, throbbing legs or a feeling of heaviness in the legs.
- Itchiness.
- Leg cramps.
- Pain that gets worse when standing and subsides when the legs are elevated.
- Pain while walking but subsides when resting.
- Thickening skin that may have the appearance of leather.
- Swelling (edema) or heaviness, especially in the lower leg and ankle.
- Tight feeling calves or painful, itchy legs.
- Varicose veins.
- Weak legs.
How is Venous Insufficiency Treated?
The goal of treating chronic venous insufficiency is to improve blood flow in the leg veins, stop the swelling, and prevent leg ulcers. Specific treatment depends on:
- The patient’s age, overall health, and medical history.
- The extent of the CVI and the signs and symptoms of the disease.
- The patient’s tolerance for specific medications, procedures, or therapies.
Most treatments for CVI are nonsurgical. In most cases, conservative treatments will improve blood flow in the leg veins. However, if the conservative measures fail to achieve the desired results, medication and non-invasive or minimally invasive procedures are available. Generally, surgery is necessary in fewer than 10 percent of chronic venous insufficiency cases.
Conservative measures that may help increase blood flow in the leg veins include:
- Wearing compression stockings to apply pressure on the legs and help blood flow. The stockings also aid in healing ulcers.
- Elevating the legs to reduce pressure in the leg veins.
- Exercise to help the body pump blood. Walking is a simple way to increase leg strength as well as boost blood flow.
- Keep legs uncrossed when sitting.
- Movement is important. Patients are encouraged not to sit or stand for a long time, if possible. If you must sit for an extended period, stretch, or wiggle your legs, feet, and ankles often to help blood flow. If you stand a lot, take breaks to sit and put your feet up to help lower pressure in leg veins.
Medication can help improve blood flow and can be used in combination with compression therapy to help heal leg ulcers. The types of medication that can help treat chronic venous insufficiency include:
- Anticoagulation therapy (blood thinners) to treat recurring problems with leg veins.
- Aspirin may be prescribed to help heal leg ulcers.
- Antibiotics can be prescribed to treat leg ulcers.
- Specific medicine (such as pentoxifylline) can be prescribed to improve the flow of blood. It may also be used in combination with compression therapy to help heal leg ulcers.
Generally, diuretics (medications used to draw excess fluid from the body through the kidneys) are not typically used to treat CVI unless additional, separate conditions (such as heart failure or kidney disease) contribute to the swelling.
Minimally Invasive Procedures
- Ambulatory phlebectomy. An outpatient procedure for removing smaller varicose veins.
- Laser therapy. A treatment using light pulses to collapse and seal damaged veins.
- Sclerotherapy. The injection of a chemical into the damaged vein so it is no longer able to carry blood. Instead, the blood returns to the heart through healthier veins.
- Subfascial Endoscopic Perforator Surgery (SEPS). This minimally invasive procedure includes the insertion of an endoscope (small, flexible tube with a light and a lens) into perforator veins. The abnormal veins are clipped and tied off, so the blood drains into healthy veins. The procedure also helps improve the healing of ulcers.
- Endovenous thermal ablation. The use of high-frequency radio waves or a laser to heat and close a problem vein.
- Catheter procedures. The insertion of a catheter (thin tube) into the vein, which is then heated and removed. The heat causes the vein to close and seal as the catheter is removed.
Surgery
Sometimes more severe cases of venous insufficiency require surgery. However, surgery is recommended in fewer than 10 percent of chronic venous insufficiency cases. Some of the surgical procedures include:
- Angioplasty and stenting. In severe cases, these minimally invasive procedures widen narrowed or obstructed veins when deep veins are affected.
- Ligation. Tying off an affected vein so that blood no longer flows through it. If the vein or valves are heavily damaged, the vein can be removed (“vein stripping”).
- Surgical repair. A vein or the valves may be surgically repaired, either through an open incision or with a long catheter (hollow tube).
- Vein bypass. This is done on veins in the upper thigh and only in the most severe cases when other procedures have failed. A healthy vein from another part of the body is used to reroute blood around the affected vein. The procedure usually requires a hospital stay of 2-5 days.
- Vein repair. Surgery to “fix” the vein or valves. It is done through an open cut on the leg or a smaller opening using a long catheter.
- Vein transplant. The transplantation of a healthy vein from another area of the body to replace a diseased vein.
Even with successful treatment, a recurrence of venous insufficiency is common and may require additional treatment.
Novus Spine & Pain Center
Dr. Torres established Novus Spine & Pain Center in Lakeland, Florida, with the goal of providing the highest quality pain management care to every patient. Whether pain is the result of an injury or from another condition, Dr. Torres offers many different treatment options.
Novus Spine & Pain Center utilizes a comprehensive approach and cutting-edge therapies to restore normal function and allow patients to regain an active lifestyle while minimizing the need for opiates. As our patient, you are our top priority. Our goal is to help you achieve the best possible quality of life.
Our Mission Statement: To provide the best quality of life to people suffering from pain by providing state-of-the-art treatments, knowledge and skill, compassion, and respect for all.
For your convenience, you may schedule an appointment online, request a call back, or call our office at 863-473-7849.
Venous Insufficiency Resources
What is Chronic Venous Insufficiency? (WebMD)
How do you know if your swollen ankles and feet are caused by venous insufficiency? (WebMD)
Skin and Sclerotherapy (WebMD)
Chronic Venous Insufficiency (Johns Hopkins)
Chronic Venous Insufficiency (Stanford Health Care)
Chronic Venous Insufficiency (Society for Vascular Surgery)
Venous Insufficiency (Healthline)
Chronic Venous Insufficiency (CVI) (Cleveland Clinic)
Venous Disease Subfascial Endoscopic Perforator Surgery (SEPS) (Cleveland Clinic)
Chronic venous insufficiency (Wikipedia)

